Healthcare organizations increasingly depend on a growing ecosystem of applications to support clinical workflows, patient engagement, and operational efficiency. At the center of this ecosystem is the electronic health record (EHR), such as Oracle Health Millennium. The challenge is not access to applications but integrating them in a way that is scalable, maintainable, and timely.
Historically, EHR integration has required significant custom development, often resulting in point-to-point interfaces that are costly to build and difficult to maintain. At the same time, traditional cloud adoption has introduced a different type of friction, including unpredictable pricing, data movement costs, and inconsistent service availability across regions.
Red Rover Health and Oracle Cloud Infrastructure (OCI) address these challenges from different layers of the stack, but with a similar objective: reducing friction that slows down innovation.
Simplifying EHR integration
Red Rover fundamentally reimagines how third-party applications connect to EHR systems. Its CORE platform provides a standardized, API-driven integration layer that enables healthcare organizations to connect “best-of-breed” applications, without building custom interfaces for every vendor relationship.
The platform uses RESTful APIs to provide secure, predictable access to EHR data, going beyond the constraints of legacy HL7 and FHIR interfaces to deliver a truly modern integration experience. Where traditional standards-based approaches still require significant custom development and ongoing maintenance, Red Rover Health eliminates that complexity, replacing point-to-point connections with a reusable, API-driven architecture built to scale with the complexity of modern health systems.
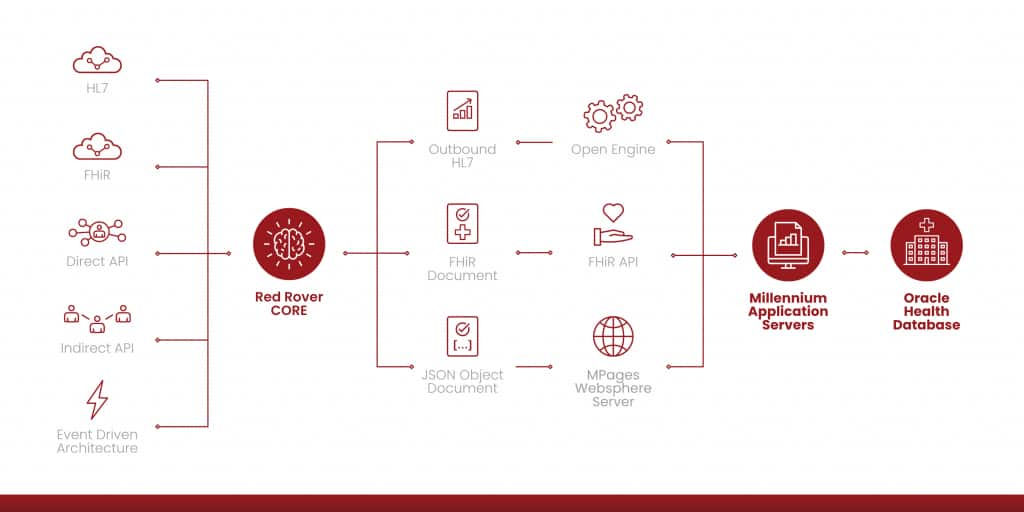
From an architectural perspective, this changes the integration model in two ways:
- Decoupled application connectivity: Third-party applications integrate once to a standardized layer rather than directly to the EHR. This eliminates fragile, one-off connections.
- Reducing integration overhead: New applications can be onboarded without repeating the same development effort for every new interface.
This model addresses a common limitation of traditional healthcare integration approaches, where even widely adopted standards may not fully support bidirectional or real-time workflows.
The result is a more modular integration architecture that accelerates the onboarding of new applications, reduces operational burden, and enables bidirectional data exchange in ways that traditional middleware cannot.
Integration as a scaling constraint
As healthcare organizations adopt more specialized applications, integration becomes a primary constraint on growth. Without a consistent integration model:
- Data remains siloed across systems
- Clinical workflows become fragmented
- Time to deploy new applications increases
Middleware platforms such as Red Rover Health shift integration from a one-off, resource intensive project to a repeatable, governed capability. This allows healthcare organizations to focus on application selection and workflow design, rather than interface development and maintenance.
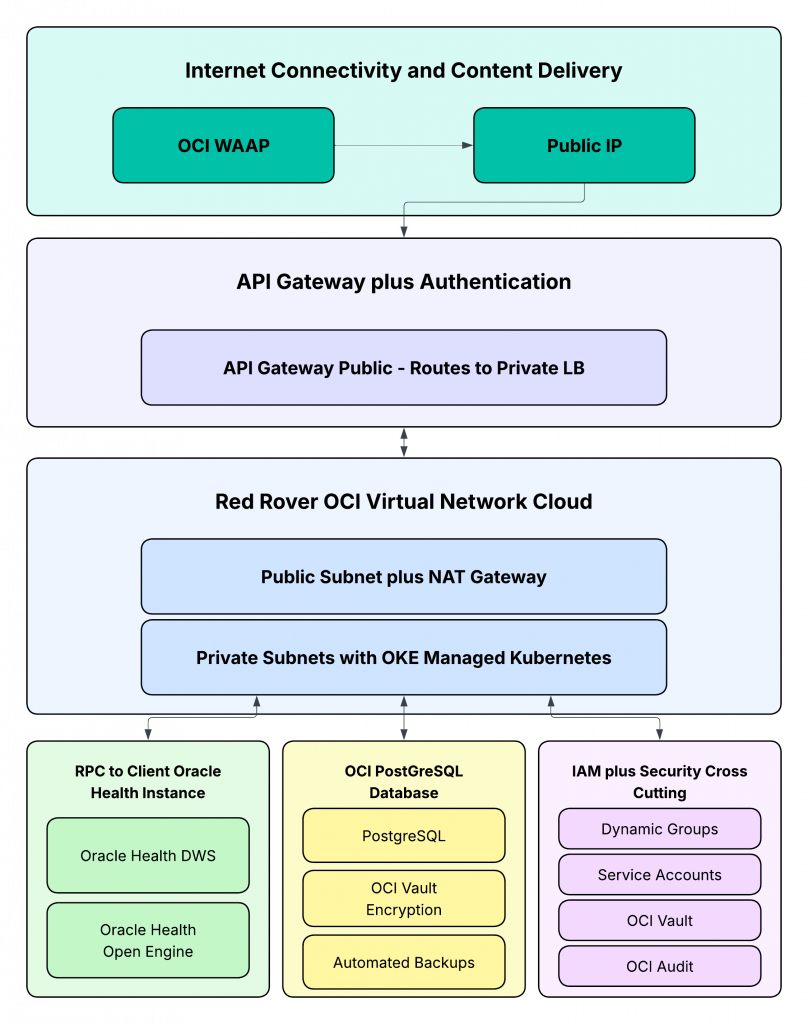
Extending the same principles to cloud infrastructure
The same types of friction visible in EHR integration often appear across cloud environments. Data gravity, pricing variability, and operational overhead can slow adoption and limit architectural flexibility. OCI, a second-generation cloud, addresses these issues through a set of architectural and commercial design choices that set it aside from first-generation cloud providers.
Eliminating data movement constraints
OCI minimizes or eliminates charges for data movement within the cloud and between different clouds with its Interconnects. This is particularly relevant in healthcare environments where data must move continuously between clinical systems, analytics platforms, and operational applications.
Removing data movement costs changes architectural decisions. Instead of optimizing for cost avoidance, organizations can optimize for:
- Data accessibility
- Real-time processing
- Cross-system integration
This aligns with the same principle seen in Red Rover Health’s integration model: reducing barriers to moving and using data.
Consistent global deployment model
OCI provides a consistent set of services across all regions. This simplifies multi-region architectures by removing the need to redesign deployments based on regional service availability.
For healthcare organizations, this consistency supports:
- Data residency requirements
- Disaster recovery architectures
- Geographic expansion
A consistent regional model also reduces operational complexity, as teams can apply the same deployment patterns globally.
Autonomous operations
OCI includes autonomous services such as Autonomous Database and Autonomous Linux, which automate tasks including patching, tuning, and security updates.
In healthcare environments, where uptime and compliance are critical, automation reduces the risk associated with manual operations and allows teams to focus on application-level functionality rather than infrastructure maintenance.
Predictable pricing
OCI uses a global pricing model with consistent pricing across regions. This reduces variability and simplifies cost planning, particularly for organizations operating across multiple geographies.
Combined with the absence of data egress penalties for many common patterns, this model allows for more predictable scaling of both workloads and data.
A common architectural outcome
Although Red Rover Health and OCI operate at different layers, their approaches result in a similar architectural outcome:
- Standardization instead of customization
- Reusability instead of point-to-point integration
- Reduced operational overhead
- Fewer constraints on data movement and system design
In both cases, removing friction enables a shift from managing infrastructure and integrations to delivering application functionality.
Enabling faster adoption of healthcare applications
For healthcare organizations, the combination of simplified integration and simplified infrastructure has a direct measurable impact on how quickly new applications can be adopted.
With a standardized integration layer, applications can be onboarded without rebuilding interfaces. With a consistent and predictable cloud platform, infrastructure does not become a limiting factor. This reduces the time between identifying a new capability and making it available to clinicians and patients.
In conclusion
Healthcare IT environments are becoming more distributed, with ever increasing numbers of applications, data sources, and integration points. In this context, complexity tends to accumulate unless it is explicitly addressed at both the integration and infrastructure layers.
Red Rover Health addresses integration complexity by providing a reusable, API-driven model for connecting applications to EHR systems. OCI addresses infrastructure complexity by reducing cost barriers, standardizing global deployment, and automating operations.
Together, Red Rover Health and OCI’s approaches support a more scalable and maintainable architecture where integration and infrastructure are no longer the primary constraints on innovation.
To learn more about how Oracle Cloud Infrastructure supports healthcare workloads or how Red Rover Health delivers Integration-as-a-Service for health systems, contact an Oracle representative or a Red Rover Health representative.
